Gum health is rarely the first thing people think about when they consider their overall wellbeing, but it probably should be. Inflamed gums have been linked to elevated systemic inflammation, heart disease, and even cognitive decline. And gingivitis, the earliest stage of gum disease, is far more common than most people expect.
Gingivitis is essentially the immune system’s response to a threat near the gum line. When plaque, a sticky layer of bacteria that forms on teeth, is not adequately removed through brushing and flossing, it accumulates and triggers an inflammatory response in the surrounding gum tissue. The reassuring part is that at this early stage, the condition is almost always reversible with consistent care and professional attention.
What makes it tricky is that gingivitis often develops without causing any pain. It can quietly progress for weeks or months before anyone notices, which is why recognizing the warning signs matters so much.
Why menopause raises gingivitis risk
Certain groups are more susceptible to gingivitis than others. People with diabetes face higher risk because elevated blood sugar creates an environment where bacteria thrive. Smokers are also at greater risk, as are people who take medications that reduce saliva production, including certain antihistamines, antidepressants, and anti-seizure drugs. Reduced saliva means reduced natural protection against bacterial buildup.
But one of the most overlooked risk factors is menopause. The reason comes down to estrogen. As estrogen levels decline during and after menopause, the salivary glands become less efficient, which reduces the mouth’s natural defenses against bacteria. Estrogen also supports bone formation and density, which means the jawbone that anchors the teeth becomes more vulnerable to deterioration over time.
Women of reproductive age face their own distinct risks. During pregnancy, surging estrogen levels can make gum tissue unusually reactive, causing it to swell and inflame in response to even minor irritation. If left unaddressed, that inflammation can advance into more serious periodontal disease. The old saying that a mother loses a tooth for every child was not entirely without basis.
Gingivitis symptoms to know
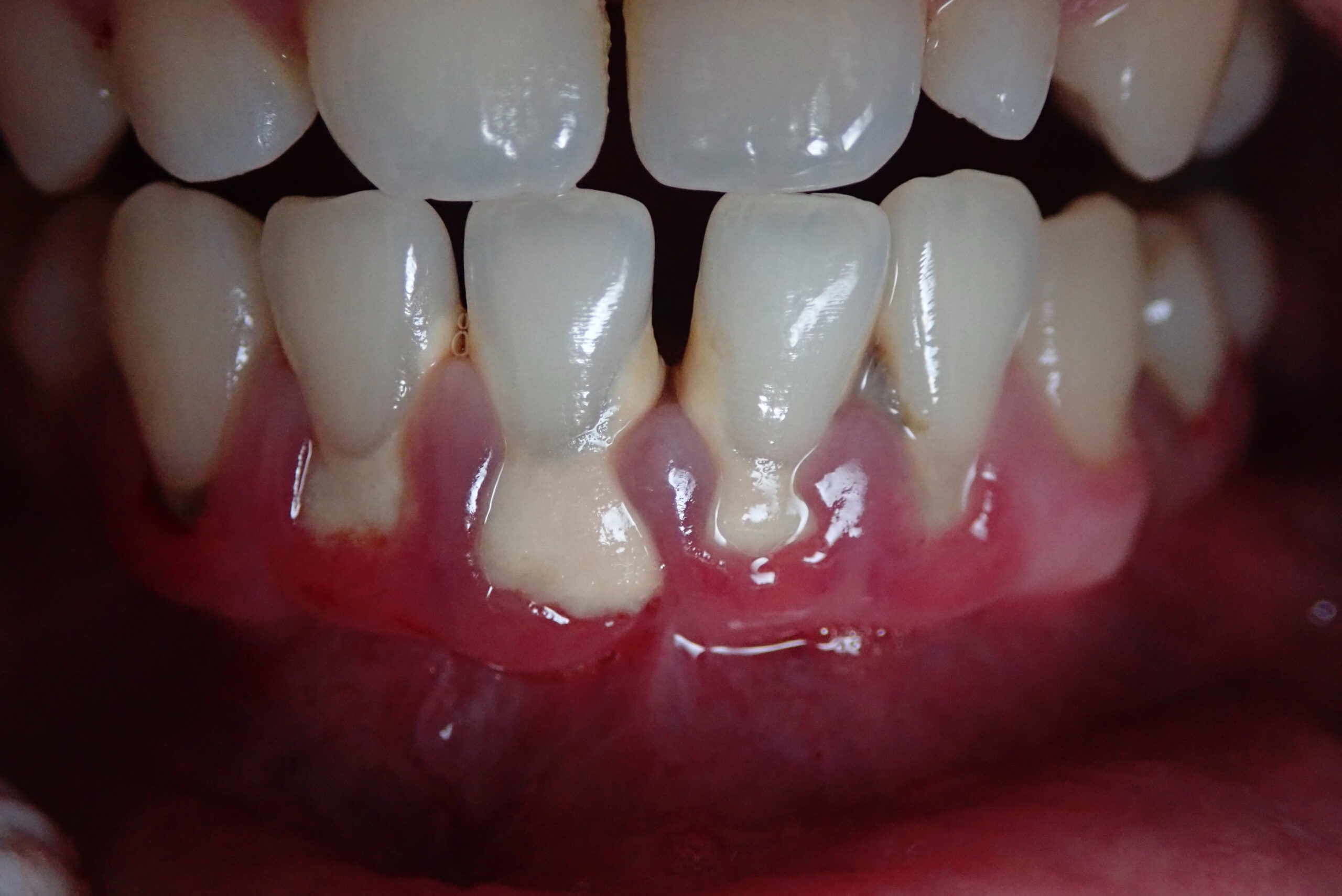
Because gingivitis tends to be painless in its early stages, it is easy to overlook the signals the body is sending. The five most common signs are bleeding gums during brushing, visible gum recession or tissue loss, swelling along the gum line, redness, and persistent bad breath.
Bleeding is the one that most people misread. The natural instinct when gums bleed during brushing is to ease up or stop, assuming the brush is being applied too aggressively. In most cases, bleeding is actually a signal that the area needs more thorough cleaning, not less. Backing off allows plaque to accumulate further and makes the inflammation worse over time.
Gingivitis and the connection to broader health
Untreated gingivitis does not stay confined to the mouth. When gum tissue remains inflamed, the bacteria responsible can enter the bloodstream and contribute to systemic inflammation throughout the body. Research has linked chronic gum disease to arterial plaque buildup and an increased risk of cardiovascular disease. For people managing diabetes, unaddressed gum disease can also make blood sugar harder to control, creating a feedback loop that worsens both conditions.
This is part of what makes early detection so important. Gingivitis caught at the right moment is not a complicated problem. It becomes one only when it is ignored long enough to progress.
How to reverse gingivitis before it goes further
The approach that dentists consistently recommend starts at home. Brushing twice a day for two full minutes using a soft-bristled brush, which can reach more effectively along the gum line and between teeth, forms the foundation. Angling the brush at roughly 45 degrees where the gum and tooth meet and using small circular motions rather than horizontal scrubbing is a technique that dental professionals point to as particularly effective.
Flossing daily removes what brushing cannot reach, which is where a significant portion of plaque tends to hide. For menopausal women especially, these habits become even more important as the mouth’s natural defenses weaken.
Professional cleanings are the other essential piece. A hygienist can remove tartar buildup that home brushing cannot address, and most early cases of gingivitis resolve within a few weeks of consistent professional and at-home care combined. For women over 50, more frequent checkups may be worth discussing with a dentist given the hormonal factors at play.
Gingivitis is common, it is often silent, and it is reversible. The key is knowing what to look for before it stops being the easier problem to solve.