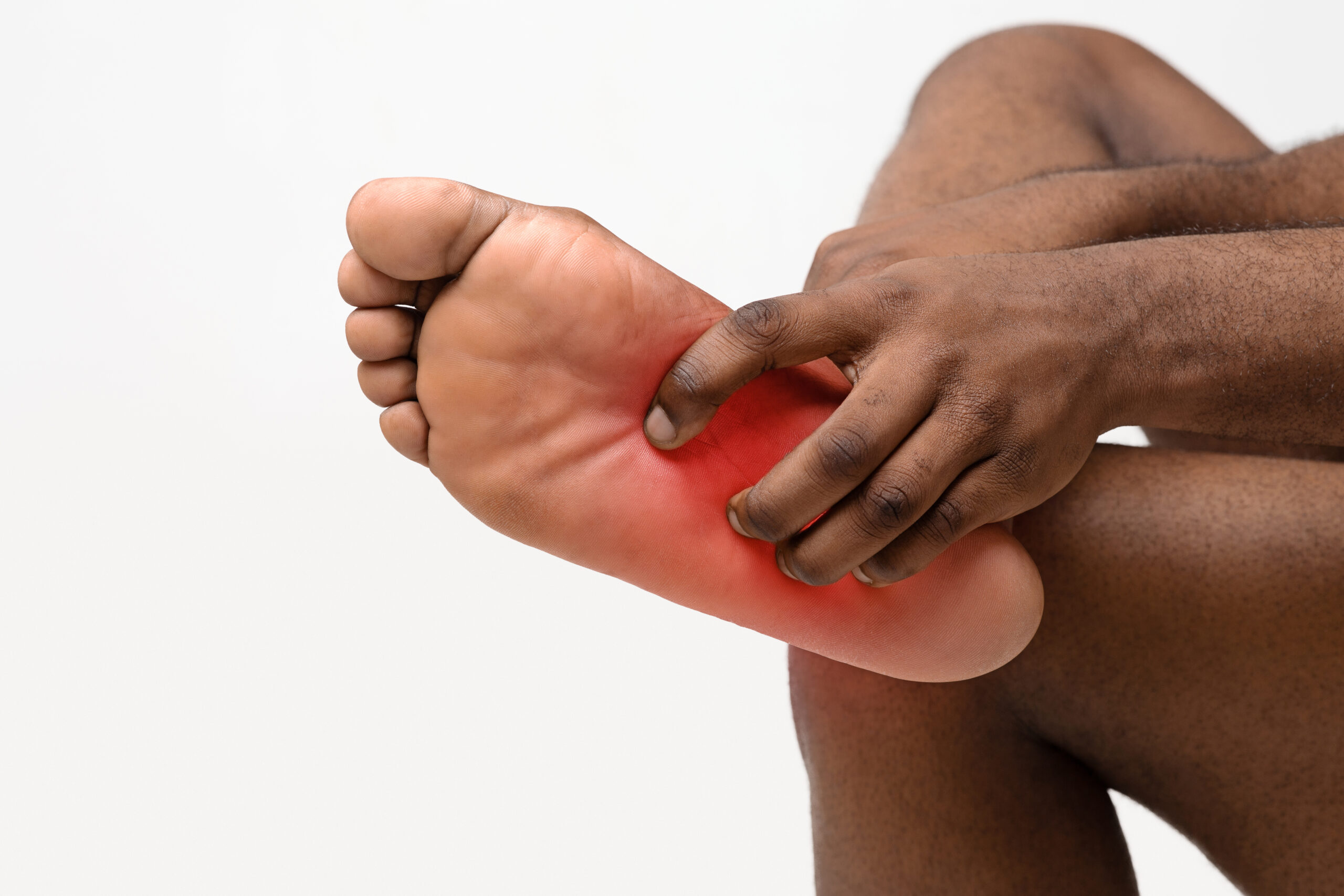
Most people who develop pain on the bottom of their foot do the same thing: they ignore it and keep moving. For a while, that strategy seems to work. Then it stops working entirely, and what began as a minor ache has become something that interferes with walking, standing, working, and sleeping. Foot pain is one of the most common physical complaints in the country, affecting up to 81 percent of people at some point in their lives. Yet despite how widespread it is, the causes are frequently misunderstood and the best paths to relief are often overlooked until the problem becomes severe.
Part of what makes this so disruptive is that it rarely stays contained. Because the feet bear the full load of every step taken throughout the day, unresolved pain at the base of the foot can alter posture and gait in ways that eventually contribute to discomfort in the knees, hips, and lower back. What starts as a localized problem can quietly become a whole-body one.
What causes pain on the bottom of the foot
The bottom of the foot is a structurally dense area containing ligaments, tendons, nerves, small joints, and cushioning fat pads, any of which can become a source of discomfort. The most frequently diagnosed cause is plantar fasciitis, a condition in which the thick fibrous band running from the heel to the toes becomes inflamed due to excessive strain or repetitive overuse. The defining symptom is sharp heel or arch pain that tends to be worst with the first steps of the morning.
Structure plays a significant role as well. Flat feet place chronic stress along the arch, while high arches concentrate pressure on the ball of the foot, a condition known as metatarsalgia. When pressure distribution is uneven over time, soreness becomes the predictable result.
Nerve-related pain is another common driver. Compression and inflammation of a nerve in the forefoot can produce pain alongside tingling or numbness, a condition known as a neuroma. Neuropathy, which presents as burning or numbness across the feet, can be a symptom of diabetes or other systemic conditions. Skin changes including corns and calluses also contribute to discomfort more often than most people account for.
Less commonly, conditions like gout, hypermobility, and rheumatoid arthritis can manifest in this area. Footwear choices compound many of these issues. Shoes that lack adequate arch support force the foot to compensate structurally, and high heels further concentrate pressure on the forefoot in ways that accelerate existing problems.
Foot pain relief and when to seek care
The good news is that most cases respond well to conservative treatment when addressed early. The first and most impactful step is footwear. Supportive shoes combined with orthotics, whether custom-made or purchased over the counter, can dramatically reduce strain and redistribute pressure. Resting when discomfort appears, applying ice to sore areas, and stretching the calf muscles, Achilles tendon, and plantar fascia are equally effective early interventions. Over-the-counter anti-inflammatory medications can help manage short-term swelling while the underlying issue is addressed.
When basic measures are not enough, physical therapy can help correct gait problems, strengthen supportive muscles, and improve overall flexibility. Corticosteroid injections or topical pain-relieving treatments may offer temporary relief while longer-term strategies take effect.
Early treatment matters in a way that is difficult to overstate. What is addressed quickly tends to resolve. What is ignored has a way of becoming structural, chronic, and eventually much harder to treat.
When to see a doctor
Pain that persists for more than a few days, makes it difficult to bear weight, or comes with visible swelling, redness, or warmth needs medical attention. Imaging such as X-rays or an MRI may be necessary to rule out stress fractures, tendon injuries, or systemic disease. Surgery is rarely required but remains an option for severe structural issues like significant bunions or tendon damage that do not improve with conservative care. The sooner a diagnosis is made, the more treatment options remain available.