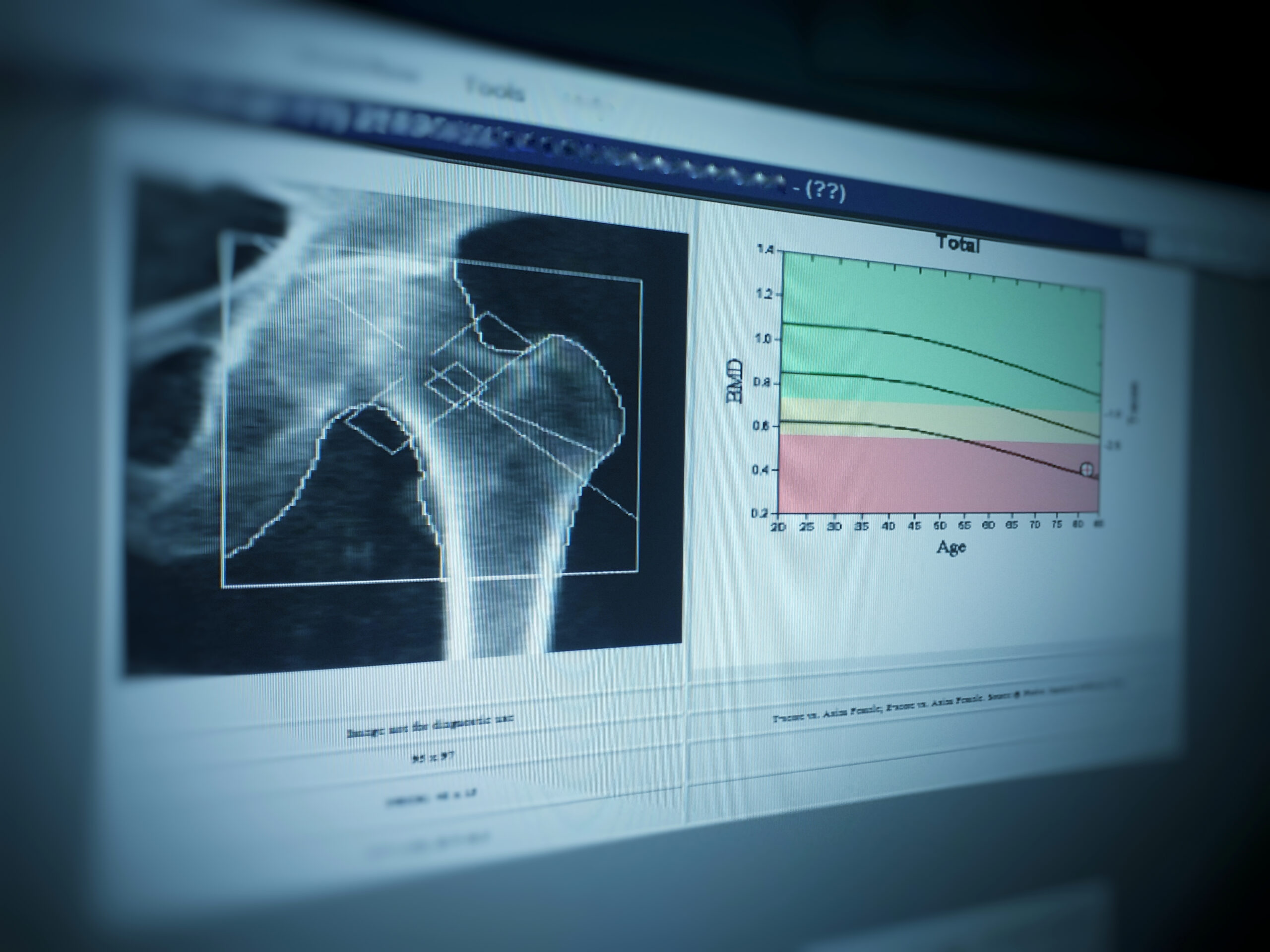
Most people associate bone loss with old age, but the reality is considerably more unsettling. Bones typically reach their peak density around age 35, and from that point forward the process of losing mass can begin, sometimes as early as a person’s 40s. For women, the transition through menopause accelerates that decline significantly, with some losing between 1 and 2 percent of their bone mass per year during the decade surrounding that shift.
Standard guidelines recommend that women begin screening for bone density at age 65, typically through a noninvasive procedure called a DEXA scan. But by that point, a woman is often several years into the bone-loss phase that follows menopause. Medical experts say that certain lifestyle, health and genetic factors can put people at meaningful risk for osteoporosis and fractures well before that age, making earlier screening worth a conversation with a physician.
Up to half of women over 50 will experience a fracture related to low bone density at some point, roughly double the rate seen in men. Many of those women did not know their bones were compromised until after the break occurred.
7 signs you may need a bone density test before 65
1. You have broken a bone with little trauma
Healthy adult bones are generally resilient enough to withstand minor everyday impacts. If you have experienced a fracture from a relatively minor incident, especially if it has happened more than once, that pattern may signal lower-than-normal bone density and merits a discussion with your doctor.
2. A close family member developed osteoporosis young
Genetics play a significant role in how well bones are built and how quickly they are lost. A parent or sibling who developed osteoporosis in their 40s or 50s, rather than later in life, suggests a possible hereditary predisposition worth screening for earlier than standard guidelines recommend.
3. You entered menopause before age 45
The earlier menopause begins, the longer the body spends with reduced levels of estrogen, a hormone that plays a critical role in protecting bone density. Early menopause can result from medical treatments, surgical removal of the ovaries or occur spontaneously, and in all cases it raises the risk of early bone loss.
4. You have been taking corticosteroids long-term
Oral corticosteroids prescribed for conditions such as asthma, lupus, rheumatoid arthritis or inflammatory bowel disease can interfere with the body’s ability to form and maintain bone tissue over time. The inflammatory conditions themselves can also contribute to bone weakening, and digestive conditions like Crohn’s disease may further impair the absorption of bone-supporting nutrients.
5. You have liver or kidney disease
Both conditions can disrupt the body’s ability to metabolize vitamin D, which is essential for calcium absorption. Kidney disease can also lead to elevated phosphorus levels that deplete calcium from the blood, while liver disease may reduce production of compounds necessary for bone formation.
6. You have a history of an eating disorder or relative energy deficiency
Relative energy deficiency in sport, a condition in which caloric intake fails to keep pace with the energy demands of athletic training, can result in very low body weight and significant bone loss. A history of disordered eating carries similar risks, as chronically insufficient nutrition takes a lasting toll on skeletal health.
7. You have recently lost a significant amount of weight
Substantial weight loss, whether through dietary changes, a GLP-1 medication or bariatric surgery, reduces the physical load placed on bones and can diminish the stimulus for new bone cell production. Research suggests that approximately 1 to 2 percent of bone mass may be lost for every 10 percent of body weight shed.
What to do if your results show low bone density
If a DEXA scan reveals below-average bone density for your age, the next step is identifying the cause alongside your physician. Genetics, underlying health conditions, long-term smoking, heavy alcohol consumption and low intake of calcium or vitamin D are among the most common contributing factors. In cases where no clear explanation exists, additional testing may be recommended.
Regardless of results, proactive habits matter. Avoiding smoking and excessive alcohol, maintaining adequate protein, calcium and vitamin D intake, incorporating weight-bearing and strength-building exercise and working on balance training can all reduce fracture risk. For those approaching menopause, hormone therapy may be worth discussing as a way to preserve bone-protective estrogen levels. In higher-risk individuals, medication may be appropriate to slow bone loss.
The earlier bone density concerns are identified, the more options exist to address them.