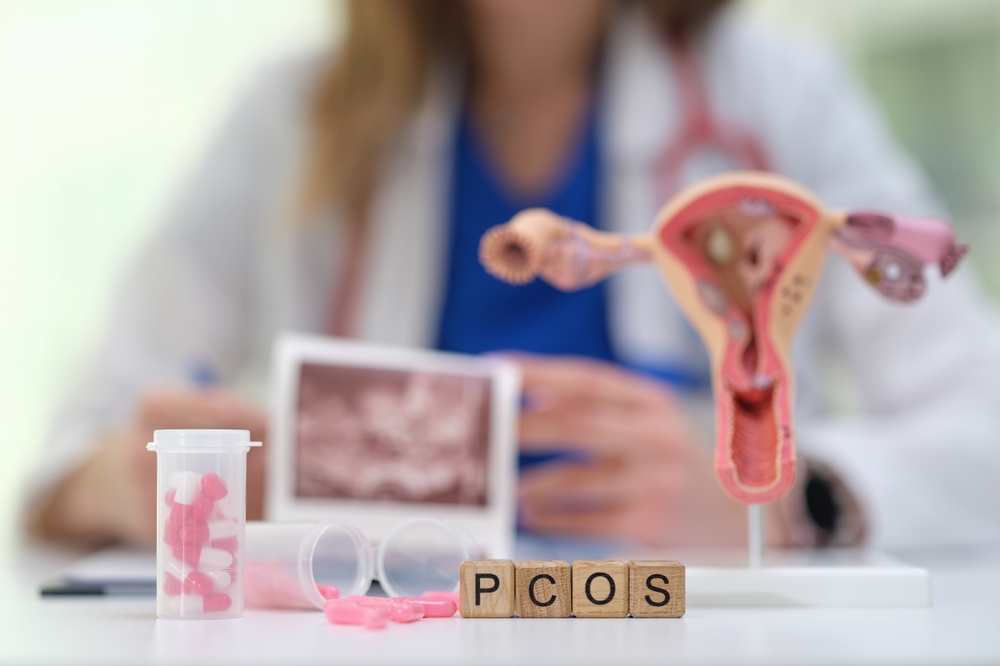
A new name for PCOS could unlock better diagnoses and long-overdue care for millions of women.
For decades, the name told only part of the story — and for millions of women, that incomplete picture came at a real cost. Now, researchers and medical experts are making a historic move to correct it.
PCOS, long known as polycystic ovarian syndrome, has officially been renamed polyendocrine metabolic ovarian syndrome, or PMOS. The change, published in the Lancet, is the result of 14 years of global collaboration involving 56 patient and professional organizations — and it signals something far bigger than a terminology update.
Why PCOS Was Always the Wrong Name
PCOS affects an estimated 10 to 13 percent of women of reproductive age worldwide. Despite that scale, roughly 70 percent of those living with the condition have never received a diagnosis, the World Health Organization reports. One of the most persistent obstacles has been the name itself.
The term polycystic ovarian syndrome pointed directly to cysts on the ovaries — a feature that does not even appear in every case. That narrow framing led to widespread confusion among both patients and providers, allowing the condition to go undetected in far too many women.
The full reality of PCOS is considerably more complex. Beyond irregular menstrual cycles and fertility challenges, the condition is now understood to carry risks for type 2 diabetes, cardiovascular disease, liver disease, sleep apnea, depression, anxiety, and body dysmorphia. It is not a reproductive disorder with a few side effects. It is a sweeping hormonal and metabolic condition that touches nearly every system in the body.
What the New Name Actually Means
The updated name — polyendocrine metabolic ovarian syndrome — was chosen with intention. The word polyendocrine shifts the framing toward what the condition actually is— a disruption in the body’s endocrine system, the chemical messenger network that regulates hormones throughout the body. When that system is thrown off balance, the consequences can be far-reaching.
Researchers now understand that elevated androgen levels, insulin resistance, and metabolic dysfunction are central features of PMOS — not secondary concerns. In the 1980s, scientists confirmed the condition’s connection to insulin resistance, revealing that the body’s inability to respond normally to insulin could eventually lead to diabetes. Since then, the list of associated conditions has only grown.
The renaming effort also aims to open doors — to more research funding, broader insurance coverage, and greater collaboration across medical specialties. Because PMOS affects so many parts of the body, no single specialty can manage it in isolation. Endocrinologists, gynecologists, cardiologists, mental health providers, and dietitians all have a role to play.
How to Get the Care You Need for PCOS
Knowing the warning signs of PMOS is the first step toward getting properly evaluated. A history of irregular menstrual cycles is one of the clearest indicators — specifically, having eight or fewer cycles per year, or cycles that stretch longer than 40 days. Symptoms like persistent acne, unexpected hair loss, or increased body hair can also point to elevated androgen levels that warrant a hormonal workup.
A physician can test for insulin resistance and androgen levels to get a clearer picture. From there, current treatment approaches generally focus on managing symptoms through a combination of lifestyle changes, medication, and specialist referrals.
A diet focused on whole foods and consistent physical activity remain the first line of recommendation. For those experiencing metabolic symptoms, certain medications — including GLP-1 medications — have shown promise, though large-scale clinical trials specific to PMOS are still limited. Hormonal birth control is commonly used to regulate cycles and reduce androgen-driven symptoms, while fertility treatments exist for those hoping to conceive.
Perhaps most critically, good PCOS care requires providers who look at the whole person — not just the symptom that brought her through the door. Fragmented care, where one specialist treats acne while another manages blood sugar and a third addresses mental health, leaves too many patients without a coherent plan. Coordinated, empathetic, individualized care is not a luxury. For those living with PMOS, it is essential.
The name has changed. The hope now is that the care follows.
Source: CNN