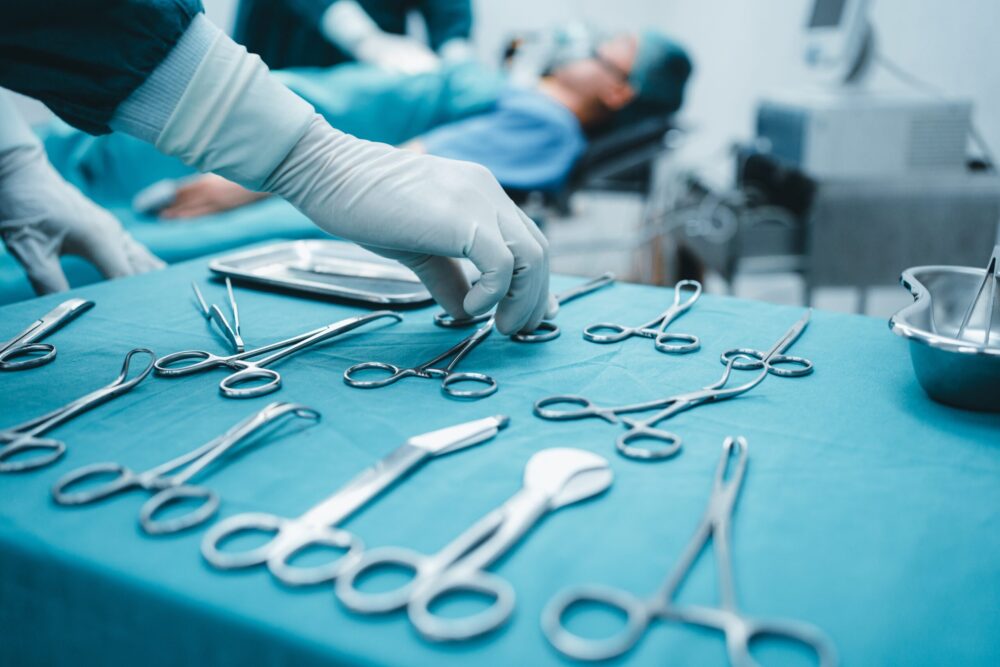
Implants are supposed to be sterile when they enter the human body. That is the most basic assumption behind every hip and knee replacement surgery performed today. But there is a moment in operating rooms that surgeons dread and rarely talk about publicly. An implant slips, hits the floor, and a split-second decision follows. Can it be cleaned and used anyway, or does the entire procedure pause while a replacement is found? That pause costs time, adds stress to an already high-pressure environment, and forces a judgment call that most surgical teams are not formally trained to make. A new study tackled that exact scenario and delivered findings that should change how surgical teams think about that decision.
Researchers evaluated what actually happens to polyethylene implant liners used in hip and knee replacement surgeries after they make contact with an operating room floor, and more importantly, whether common disinfectants can make those implants safe again. The study was conducted across four orthopedic operating rooms and included more than 200 implant liners tested under conditions designed to reflect real surgical situations. The results were sobering.
Implants and the bacteria hiding on OR floors
Operating room floors are not clean. That statement might seem obvious, but the extent of contamination documented in this research is striking. Floor samples collected from surgical sites showed a median bacterial count in the thousands, and every single sample tested positive for microbial growth. There were no exceptions.
Among the pathogens identified, Enterococcus bacteria appeared in nearly all samples. Strains of Staphylococcus aureus, including the drug-resistant form known as MRSA, were found in a significant share of samples, and Gram-negative bacteria turned up in nearly two thirds of tested sites. These are not minor organisms. They are the kinds of bacteria directly linked to serious joint infections after surgery, infections that can require additional procedures, prolonged hospital stays, and in some cases, removal of the implant entirely.
When the study team placed implant liners on those floors for just 10 seconds, the liners picked up measurable bacterial contamination before any disinfection was attempted. The floor-to-implant transfer was immediate and consistent.
Implant disinfection works, but not with alcohol
The study tested three disinfectant approaches against an untreated control group. Chlorhexidine-alcohol and povidone-iodine both produced meaningful reductions in bacterial load and outperformed the control group by a significant margin. Ethanol, which many surgical teams reach for instinctively in high-pressure moments, did not.
Ethanol failed to achieve a statistically significant reduction in bacteria compared to doing nothing at all. When looking specifically at hip implant liners, only the chlorhexidine-alcohol and povidone-iodine treatments showed meaningful results. Ethanol fell short across multiple measures and came in significantly behind both of the other options tested.
Even among the implants treated with the two more effective solutions, the news was not entirely reassuring. Neither chlorhexidine-alcohol nor povidone-iodine achieved full sterility. More than one in six treated implants still carried clinically important pathogens after disinfection. That residual risk is not something that can simply be accepted and moved on from. The bacteria that remained were not harmless background organisms either. They included the same strains most closely associated with deep joint infections, the kind that can derail a patient’s recovery for months or longer.
The case for replacing a dropped implant
The clearest takeaway from this research is that replacing a dropped implant remains the safest and most defensible choice. When a replacement is genuinely not available, chlorhexidine-alcohol or povidone-iodine immersion represents the best available rescue option, but it is a backup plan, not a solution. Thinking of it as anything more than that would be a mistake, and this study makes that boundary very clear.
What the study also makes visible is the absence of any standardized protocol guiding surgeons through this exact situation. Right now, the decision is largely left to individual judgment in the middle of a procedure, under pressure, without a clear institutional playbook to follow. That variability is a problem. Two surgeons in the same hospital might handle a dropped implant in completely different ways, and neither of them would be acting outside the current standard of care simply because no such standard exists yet.
Patients who experience an implant drop during their surgery deserve to be informed, and they deserve to be monitored closely for signs of infection in the weeks that follow. Periprosthetic joint infections are among the most serious complications in orthopedic surgery, and even a small increase in risk tied to a preventable event is worth taking seriously. As surgical teams and hospitals process these findings, the next step is building consistent, evidence-based guidelines so that the right call is never left to chance.