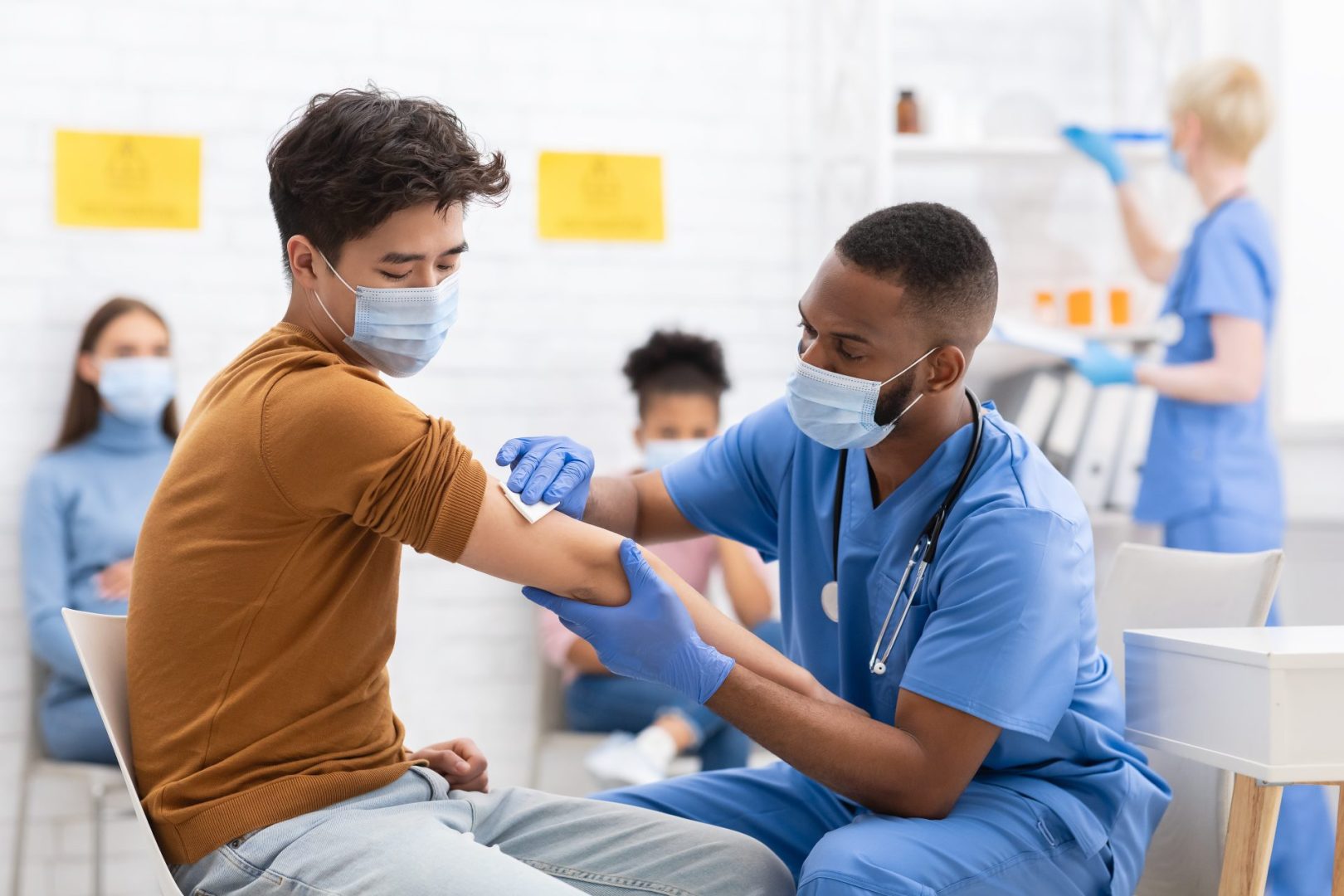
Just as warmer weather begins to lift spirits, a new COVID-19 variant is making its way across the country and bringing plenty of uncertainty with it. Known informally as the cicada variant, this strain is believed to be an Omicron subvariant sometimes associated with BA.3.2, though it carries no official designation from the Centers for Disease Control and Prevention or the World Health Organization. Despite its unofficial status, health experts are paying close attention to the way it spreads and how it interacts with immunity people already have.
What makes the situation more challenging is the current state of national surveillance. The United States does not have a real-time system for tracking COVID-19 symptoms at scale, which means the full picture of how widely this variant is circulating remains unclear. That absence of data is not the same as reassurance, and health professionals are urging the public to stay alert rather than assume the coast is clear.
Cicada variant symptoms to watch for
The good news, if there is any, is that the cicada variant does not appear to come with an entirely new set of symptoms. Most people who contract it report the same range of discomforts associated with recent Omicron-family strains. Those include sore throat, cough, fatigue, fever, chills, headache, congestion, runny nose and body aches.
Most cases remain mild and resolve without medical intervention. However, symptoms like difficulty breathing or chest pain should prompt immediate medical attention, even in people who consider themselves otherwise healthy. Severe cases can and do occur outside of high-risk groups, and no one should dismiss early warning signs.
It is also worth remembering that even mild infections carry a risk of long COVID, a condition whose full effects are still being studied but whose impact on daily life can be significant and lasting.
What makes this variant different
The cicada variant does not necessarily feel different from earlier strains once you are sick, but it may be more likely to infect you in the first place. The key distinction researchers are watching is its apparent ability to partially evade immunity built up through prior infection or vaccination. That means people who felt protected after previous exposure may find themselves more vulnerable than expected.
That said, there is currently no evidence that the cicada variant causes more severe disease or leads to meaningfully different clinical outcomes compared to other recent strains. The concern is primarily about its transmissibility and its relationship to existing immune defenses, not a dramatic shift in how sick it makes people.
Do vaccines still offer protection
Current COVID-19 vaccines, including the updated formulations for the 2025 to 2026 period, were designed with the JN.1 lineage in mind. The variants most actively circulating right now, including XFG and NB.1.8.1, fall within that lineage, which means the existing vaccines still provide meaningful protection against severe illness. The cicada variant, linked to BA.3.2, is expected to follow a similar pattern.
Vaccines may be less effective at fully preventing infection given the variant’s ability to sidestep some antibody responses, but they remain the strongest tool available against hospitalization and serious outcomes. For the roughly 90 million Americans living in states where BA.3.2 has already been detected, getting up to date on vaccination is a practical and evidence-based step, not a speculative one.
Beyond vaccination, familiar protective habits still apply. Masking in crowded indoor spaces, testing when symptoms appear, isolating after a positive result and washing hands frequently all remain effective. Maintaining a healthy routine including quality sleep, regular movement, a nutrient-rich diet and managed stress levels also supports the immune system’s ability to respond.
Does COVID slow down in warmer months
Spring and summer do not guarantee a reprieve from COVID-19. Unlike influenza, which follows a fairly predictable seasonal arc, COVID-19 has surged across every season and does not reliably slow down when temperatures rise. Improved outdoor ventilation can help, but open windows are not a substitute for other precautions.
A strong summer wave can sometimes reduce the virus’s immediate momentum heading into fall, but that pattern breaks down whenever a new variant enters circulation and resets the conditions. Forecasting based on the season alone has consistently proven unreliable.
How to recover if you test positive
If you test positive, treating the cicada variant the same way you would any recent COVID strain is the recommended approach. Over-the-counter medications like acetaminophen or ibuprofen can ease fever, body aches and headache. Saline nasal sprays help with congestion, and honey or throat lozenges offer some relief for cough and soreness.
Rest and hydration are two of the most underrated recovery tools available. Fluids including water, electrolyte drinks, warm tea, broth and soup are especially important if fever, vomiting or diarrhea are present. Antiviral medications are worth asking about early, ideally within the first five days of symptoms, particularly for older adults, pregnant people and those living with conditions like diabetes, obesity or heart, lung or kidney disease.